13 min read
May 31, 2026
Fertility Preservation in Australia: Egg, Embryo and Sperm Freezing Options
Written by
Fertility2Family Team

Medically reviewed by
Evan Kurzyp, RN, BSN, Master of Nursing
AHPRA registration: NMW0002424871
Fertility preservation gives people in Australia the option to have children in the future even if age, illness, or medical treatment may affect fertility. It covers established methods such as freezing eggs, embryos, and sperm, along with options like ovarian tissue storage in selected cases. Awareness has grown as more Australians learn how fertility changes with age and how cancer therapy, endometriosis surgery, or gender-affirming care can reduce reproductive potential. Preservation is delivered at specialist fertility clinics in Australia and around the world, and it is often time sensitive. The aim is to plan ahead, match the method to your health and life goals, and understand the likely outcomes and costs. This guide explains what to expect, when to seek help, and how home tools like ovulation and pregnancy tests fit into that picture in Australia.

Quick Answers About Fertility Preservation
What is fertility preservation? It is the planned freezing of eggs, embryos, sperm, or reproductive tissue for later use. It supports people delaying pregnancy, those with low ovarian reserve, cancer patients, and others at risk of reduced fertility.
Who should consider it? Consider preservation if you are about to start cancer therapy, need ovarian or testicular surgery, have a family history of early menopause, plan to delay pregnancy, or are starting gender-affirming treatment. A GP or fertility specialist can tailor advice.
How much does it cost in Australia? Costs vary by clinic and method. Egg freezing often ranges from five to ten thousand dollars per cycle with extra for medications and storage. Embryo freezing may be higher. Sperm freezing is far cheaper. Medicare rebates may apply in medically indicated cases.
What Is Fertility Preservation in Australia
Fertility preservation is the process of storing reproductive cells at low temperatures so they can be used later. Clinics use vitrification for eggs and embryos, which helps protect cells during freezing and thawing. Sperm freezing uses liquid nitrogen. In some cases surgeons remove and freeze ovarian tissue so that follicles can be reimplanted later. Care is delivered by fertility specialists in Australia, including large centres such as IVF clinics. Many clinics offer streamlined oncofertility pathways when timing is tight before chemotherapy or radiotherapy.
Egg freezing can suit someone who is not ready to fertilise eggs with sperm now. Embryo freezing may suit a couple who are ready to combine eggs and sperm before treatment, which allows the laboratory to assess embryo quality. Sperm freezing provides a simple, fast option for male preservation. These services are available across Australia and many clinics share results data and protocols with peers across Australia and around the world to maintain best practice.
Preservation does not guarantee a future pregnancy. It provides a chance to try assisted reproductive treatment later. Outcomes depend on age, number and quality of eggs or embryos, menstrual health, sperm quality, and clinic expertise.
Who Might Consider It, Why, and When to See a GP
People consider preservation for medical and personal reasons. Medical reasons include cancer therapy that could harm the ovaries or testes, surgery for ovarian cysts or endometriosis, or conditions such as severe endometriosis where ovarian reserve may fall faster. A family history of early menopause can also motivate earlier planning. Transgender people often freeze eggs or sperm before starting hormones or surgery that can impair fertility.
Personal reasons include wanting more time to meet the right partner, study, career goals, or current life circumstances. Because egg quality falls with age, earlier preservation usually leads to a better pool of eggs. For men, sperm quality can also decline with age and health conditions, though usually more gradually.
See your GP or a fertility specialist promptly if you are about to start cancer therapy, if you have been advised to have ovarian or testicular surgery, if you are under 35 and plan to delay pregnancy for several years, if you are over 35 and concerned about ovarian reserve, or if you are considering gender-affirming treatment. Do not delay if a treating team has set a date for chemotherapy or radiotherapy. Early referral gives more planning time and often improves options.
Assessment and Testing in Australia
The usual pathway starts with a GP referral to a fertility specialist. The first consult covers medical history, menstrual cycles, medications, prior pregnancies, and lifestyle. The specialist will outline options and timelines and request tests to guide the plan.
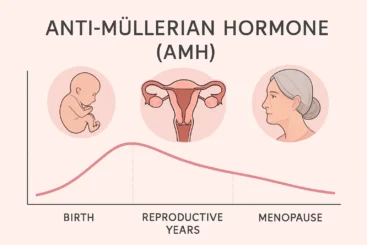
For women, testing often includes anti-Müllerian hormone, which estimates ovarian reserve, and transvaginal ultrasound to assess antral follicle count and overall pelvic health. Blood tests may check FSH, LH, oestradiol, thyroid function, and prolactin. Screening for infections is routine before storage. Some people consider genetic carrier screening. These tests help predict egg yield and the best stimulation approach for egg collection.
For men, semen analysis checks volume, count, movement, and shape of sperm. Blood tests screen for infections. If ejaculated sperm are not available, a urologist may discuss surgical retrieval from the testes. A plan is then set for freezing multiple samples to maximise future options.
People facing cancer treatments often meet a fertility specialist within days. Oncofertility pathways coordinate with oncology teams so fertility procedures fit safely around chemotherapy or surgery dates. Your hospital team and fertility clinic communicate to avoid delaying cancer care.
What the Procedures Involve for Women and Men
Egg freezing starts with ovarian stimulation. You self-inject hormone medication for around ten to twelve days while the clinic monitors follicles with ultrasound and blood tests. When follicles are ready, a trigger medication matures the eggs. The egg collection is a short procedure under sedation. A thin needle passes through the vaginal wall into the ovaries to collect eggs. The laboratory assesses eggs and freezes suitable mature eggs.
Embryo freezing follows the same steps to retrieve eggs. The laboratory then fertilises eggs with sperm to create embryos. Embryos grow in culture for several days. Viable embryos are vitrified for storage. Because fertilisation has already occurred, this method can provide more information about embryo quality at the time of freezing.
Ovarian tissue preservation is considered when there is not enough time for stimulation or for prepubertal girls. A surgeon removes a small piece of the ovarian cortex by keyhole surgery. The tissue is frozen in small strips. Later in life, it may be transplanted back to the pelvis to restore hormone function and the chance of pregnancy. It is not suitable for all cancers because there is a small risk of reintroducing cancer cells, so oncology input is essential.
Sperm freezing is straightforward. A semen sample is produced on site, then processed and frozen in multiple vials. If needed, a urologist can retrieve sperm surgically. Men can usually provide more than one sample across several days to build a larger stored supply.
Testicular tissue freezing for prepubertal boys is still developing. In adults with no sperm in the semen, surgical retrieval can help. These decisions are made with a specialist and, for children, with a paediatric team.
Procedures are delivered at Australian fertility clinics such as IVF centres in capital cities and regional hubs. Many clinics publish clear step by step guidance. See local clinic pages for details such as the egg freezing pathway.
At Home Steps That Support Reproductive Health
Daily habits can support fertility and treatment outcomes. If you smoke, quitting improves ovarian and sperm health. High alcohol intake can disturb hormones and ovulation. Aim for light to moderate intake and avoid alcohol when taking fertility medication or if pregnant. Regular physical activity supports overall health. Very intense training can stop periods for some women and can reduce sperm quality for some men, so balance is important. If weight is above or below the healthy range, gradual changes through diet and exercise can improve hormone balance and outcomes in treatment.
Stress can disrupt cycles and sleep. Simple steps such as a regular bedtime, short daily walks, mindfulness practice, or counselling can reduce symptoms. Fertility counselling is available through Australian clinics and through the Australian and New Zealand Infertility Counsellors Association directory. If anxiety or low mood is present, a GP can provide a mental health plan and refer to psychology.
Some people use acupuncture during treatment. Choose a practitioner registered with the Chinese Medicine Board of Australia through AHPRA. Evidence is mixed, so set realistic expectations and coordinate with your fertility specialist about timing around egg collection or embryo transfer.
Nutritional supplements such as myo-inositol or Coenzyme Q10 are used by some patients preparing for stimulation. Products listed with the Therapeutic Goods Administration include a label with an AUST L number. Always discuss supplements with your fertility doctor or a registered dietitian, especially if you take other medicines. A personalised plan reviewed every few months helps avoid unnecessary products.
At home ovulation tests and pregnancy tests can help you understand timing and reduce uncertainty. Ovulation tests detect the LH surge that precedes ovulation by around one to two days. Pregnancy tests detect hCG in urine from the first missed period. Fertility2Family offers reliable ovulation and pregnancy tests that many Australians use to track cycles before and after treatment. Home tracking is not a substitute for clinic monitoring, but it can support cycle awareness between appointments.
Costs, Rebates, and Access Across Australia
Prices vary by clinic and city. As a guide, a single cycle of egg freezing often costs between five and ten thousand dollars, not including medications and storage. Embryo freezing can cost eight to fifteen thousand dollars per cycle. Ovarian tissue preservation can cost fifteen to twenty thousand dollars. Sperm freezing is commonly five hundred to one thousand dollars. Surgical sperm retrieval and testicular tissue storage can be higher, often in the fifteen to twenty thousand dollar range. Ongoing storage fees apply each year.
Medicare rebates may apply when fertility is at risk from medical treatment. Some hospital costs for procedures done in a private hospital may be covered by private health insurance policies that include fertility or theatre fees. Coverage varies, so speak with your insurer before you book. Item numbers on the Medicare Benefits Schedule apply to some steps in care, which can reduce out of pocket costs.
Public hospitals in some states provide urgent oncofertility support, particularly for young people with cancer. Your oncology team and hospital social worker can advise on local services, travel support, and any grants. Clinics usually have finance teams who can give written quotes that include storage fees and any expected rebates. Ask for a full breakdown so you can plan.
Success Rates and Medical Risks
Outcomes depend on age, reproductive health, the number of eggs collected, embryo quality, sperm quality, and the processes used in the laboratory. Freezing eggs at a younger age generally offers a higher chance of a baby per egg. Embryo freezing can provide higher certainty at the time of freezing because fertilisation has already occurred, although future outcomes still vary. Sperm freezing has a long track record with good survival after thawing when handled in accredited laboratories. Ovarian tissue reimplantation has helped many patients restore hormone cycles and some achieve pregnancy, though it is not suitable for every diagnosis.
Risks for women include discomfort during stimulation, bloating, temporary mood changes, and bruising from injections. Ovarian hyperstimulation syndrome has become less common with modern medication protocols but can still occur and needs monitoring. Egg collection carries small risks of bleeding, infection, and anaesthetic side effects. For men, sperm banking is low risk, while surgical retrieval has minor surgical risks such as bruising and swelling.
No fertility preservation method guarantees a future pregnancy. The Fertility Society of Australia encourages clinics to report outcomes and use quality systems so patients receive clear, realistic guidance. Your specialist will discuss likely scenarios for your age and health and will suggest how many cycles or eggs might be needed to reach your goals.
Frequently Asked Questions About Fertility Preservation Australia
How long can eggs, embryos, and sperm stay frozen? Storage can continue for many years in Australia. Clinics will ask you to renew consent and storage each year. There is no set expiry for cell viability, though outcomes relate to the age at freezing.
Does egg freezing delay menopause? No. Egg collection does not change the timing of menopause. It reaches into the pool of eggs that would have been lost that month and does not deplete the overall supply.
Can I work during an egg freezing cycle? Most people keep working. You will have several morning appointments for blood tests and ultrasound. Allow time off on the day of egg collection and avoid strenuous activity until cleared by your clinic.
Is preservation safe if I have PCOS? Many people with polycystic ovary syndrome undergo egg freezing safely with tailored medication. The clinic uses protocols that lower the chance of ovarian hyperstimulation. Close monitoring is standard.
Can I create embryos now using donor sperm? Yes. Australian clinics follow strict laws and consent. If using donor sperm, the clinic will guide you through screening, counselling, and legal steps before creating and freezing embryos.
What happens if I move interstate or overseas? Clinics can transfer frozen eggs, embryos, or sperm between accredited centres. The logistics and fees vary. Speak with your clinic well in advance to arrange safe transport.
Ready to Take the Next Step
If you are thinking about preserving your fertility, start with a clear plan that fits your health, timeline, and budget. Book a chat with your GP to arrange a referral and initial tests. If you are facing cancer treatment, ask your oncology team for an urgent oncofertility referral and let your fertility clinic know your treatment dates. Bring questions about expected egg numbers, how many cycles may be needed, success rates for your age, clinic reporting, and total costs including storage. If you are considering donor sperm, genetic screening, or future single parenthood, ask about counselling and legal steps so your plan is well set up.
Between appointments, simple tools can help you stay informed and calm. Many Australians use Fertility2Family ovulation test strips and pregnancy test strips to track cycles before and after preservation. If you are making lifestyle changes, take small, steady steps and use support from your GP, a dietitian, and an ANZICA accredited counsellor. Good care draws on trusted information, skilled clinical teams, and your values. With a tailored plan, you can protect options for a future family in a way that feels right for you.
Last reviewed: May 2, 2026
Next scheduled review: Mar 2027
References
Fertility2Family publishes Australia-focused fertility education. Articles are written by our team and medically reviewed by Australian-registered health practitioners. We use Australian consumer medicine information, Australian clinical and public health guidance, and peer-reviewed research consistent with Australian care. We explain what the evidence suggests, what it cannot confirm, and when to see a GP or fertility specialist. Each article lists its author, medical reviewer, and review dates.
https://www.healthdirect.gov.au/infertility
https://www.healthdirect.gov.au/ivf
https://www.fertilitysociety.com.au
https://www.racgp.org.au/clinical-resources
https://ranzcog.edu.au/patient-information
https://www.jeanhailes.org.au/health-a-z/fertility
https://www.cancer.org.au/cancer-information/treatment/side-effects/fertility
https://www.betterhealth.vic.gov.au