
11 min read
May 31, 2026
AMH Levels and Fertility: What Low AMH Means
Written by
Fertility2Family Team

Medically reviewed by
Evan Kurzyp, RN, BSN, Master of Nursing
AHPRA registration: NMW0002424871
Trying to conceive can feel uncertain when advice is mixed and timelines vary. Many Australians come across the anti-mullerian hormone test when looking for answers about fertility. Anti-mullerian hormone, often called AMH, is made by cells in the ovarian follicles. A simple blood test estimates your current ovarian reserve, which means the number of eggs likely to be available at that point in time. AMH is not a pregnancy test and it does not predict egg quality or guarantee success with treatment. It is one piece of a wider fertility picture that includes age, menstrual history, ultrasound findings, and partner factors. This guide explains what AMH is, what your result can and cannot tell you, how testing works in Australia, and when to see a GP or specialist. It also covers practical steps you can take at home and how ovulation and pregnancy tests fit into day to day planning.
Quick Answers About Anti-mullerian Hormone (AMH)
What does an AMH test show?
AMH reflects your current ovarian reserve. Higher levels usually mean more available eggs, while lower levels suggest fewer. It does not measure egg quality or predict natural pregnancy on its own.
When should I test AMH in Australia?
You can test any day of your cycle because AMH is relatively stable. A GP or fertility specialist can order the test, and some private pathology services accept referrals for self-requested blood tests.
Does a low AMH mean I cannot get pregnant?
No. Low AMH indicates a smaller egg supply, not zero chance. Many people conceive naturally or with help. Age, sperm health, uterine factors, and treatment choices also influence outcomes.
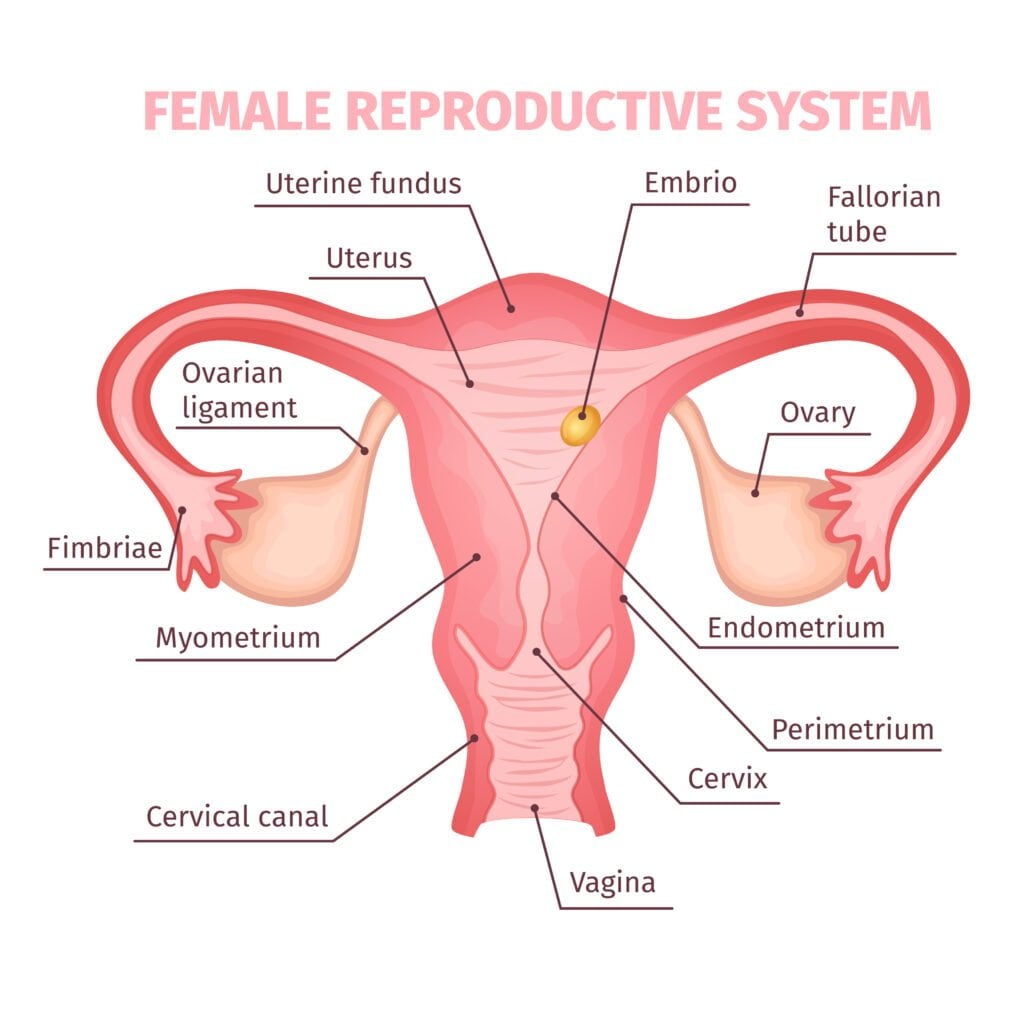
What is AMH and how it works in the body
Anti-mullerian hormone is a protein made by cells in small ovarian follicles. In males and females, AMH plays a role during early development. In females after puberty, AMH reflects the pool of growing follicles in the ovaries. It is different from pregnancy hormones such as hCG and from sex hormones like progesterone. AMH is not a cycle day tracker. Rather, it helps estimate ovarian reserve, sometimes called the ovarian reserve. Levels tend to be higher in younger adults and trend lower with age. The reading is one part of a wider assessment that can include ultrasound of the ovaries, cycle history, and partner testing. Understanding its limits helps you use the result to plan next steps without unnecessary worry.

What affects AMH levels and why they vary
AMH usually declines with age as the number of follicles reduces. Individual rates of change differ due to genetics and health history. Ovarian surgery, chemotherapy, and pelvic radiation can lower AMH by reducing follicle numbers. Smoking is linked with faster ovarian ageing, while maintaining a healthy weight and treating endocrine conditions can support stable hormonal patterns. Hormonal contraception may slightly change readings in some people. Pregnancy can temporarily lower AMH without long term meaning. Elevated AMH can occur with polycystic ovary syndrome due to a higher count of small follicles. A single result should be read alongside cycle history and ultrasound, often with an antral follicle count. If a reading is unexpected for your age or symptoms, a repeat test and review with your GP or specialist can confirm the pattern before any decisions.
How AMH testing works in Australia
AMH is measured with a standard blood test. A clinician cleans the skin, draws a small blood sample from a vein in your arm, and sends it to a pathology lab for analysis. No fasting is needed. The test can be done on any day of your menstrual cycle. Most people feel only brief discomfort at the needle site. The result is usually reported in nanograms per millilitre. In Australia, Medicare does not routinely cover AMH when ordered on its own, although your GP can advise on rebates when the test forms part of a broader fertility work up. Fees vary by provider and location. Many Australians pay between seventy and one hundred and fifty dollars out of pocket. Your local clinic or pathology provider can confirm current pricing and whether a referral is required. For more on collection processes, see Clinical Labs.
What AMH results can and cannot tell you
AMH helps estimate how many eggs remain in your ovaries at the time of testing. A common reference range for adults is about 1.0 to 3.0 ng/mL. Readings below 1.0 ng/mL are often described as low. Values near 0.4 ng/mL suggest a very small remaining pool. These thresholds are guides rather than strict cut-offs, and the same number can carry different meaning at age 25 compared with age 40. Laboratories use different assays, so small differences between services are normal. AMH does not measure egg quality. It does not predict natural conception by itself. It does not set the day you will reach menopause, although very low results can align with perimenopause. It is most useful when considered with age, menstrual patterns, ultrasound findings, and semen analysis. A fertility specialist can place your AMH in context and advise whether repeat testing adds value.
AMH, infertility and the role of IVF
When someone has trouble conceiving, AMH helps clinicians plan treatment. Lower AMH often means fewer follicles will respond to ovarian stimulation in an IVF cycle, which can lead to fewer eggs collected. Success in IVF depends on several steps including egg quality, fertilisation, embryo development, and uterine receptivity. People with low AMH still achieve pregnancies, although more than one cycle may be needed. High AMH may suggest polycystic ovary syndrome. In that case, care may focus on improving ovulation patterns and reducing risks such as ovarian hyperstimulation during treatment. Diagnosis of PCOS relies on a mix of symptoms, androgen levels, and ultrasound findings, not AMH alone. If your AMH is outside the expected range for your age or history, your GP can arrange an early referral to a reproductive endocrinologist for targeted advice.
Home management and practical steps while you plan
There is no proven way to directly raise AMH because it reflects egg supply rather than a hormone that can be trained upward. You can support reproductive health with steady habits. Aim for regular sleep and a routine that eases stress. Keep alcohol intake within Australian guidelines and avoid smoking. Work with your GP on weight management and nutrition that suits your body and any underlying conditions such as thyroid disease or insulin resistance. Some people discuss supplements such as vitamin D or coenzyme Q10 with their clinician. Evidence for AMH change is limited, though general health measures often support cycle regularity and preconception care. If you are trying to conceive, track your fertile window and consider preconception screening, rubella immunity checks, and folic acid. Good planning cannot add eggs, but it can help you use the fertile days you have.
When to see a GP or specialist in Australia
See your GP if you are under 35 and have been trying for 12 months without pregnancy. If you are 35 or older, seek advice after 6 months. Go sooner if your periods are very irregular or absent, if you have severe pelvic pain, known endometriosis, a history of pelvic surgery, or if chemotherapy is planned. Your GP can arrange first line tests including AMH, follicle stimulating hormone, thyroid function, prolactin, and a pelvic ultrasound that includes an antral follicle count. Your partner may need a semen analysis. Depending on the findings, you may be referred to a fertility specialist. Australians can access public hospital fertility clinics in some states, though waiting times vary, or choose private clinics for faster access. Use Healthdirect and state health services to locate local pathways and support.
How ovulation and pregnancy tests fit with AMH
AMH does not tell you when you ovulate. Ovulation predictor kits measure luteinising hormone in urine to identify the fertile window in the current cycle. This is helpful if you have a smaller ovarian reserve and want to time intercourse or insemination accurately. Pregnancy tests measure hCG in urine to confirm pregnancy after a missed period. Both tools support day to day planning while AMH guides overall expectations. If timing is your main challenge, using high sensitivity ovulation tests can shorten the guesswork each month. When you miss a period or reach the end of the luteal phase, accurate pregnancy tests can confirm results without delay. For questions about test choice or how to read lines, visit our fertility advice hub or contact the team for guidance on product use alongside your medical plan.
Frequently Asked Questions About Anti-mullerian Hormone (AMH) Australia
Can I test AMH while on the pill
Yes. AMH can be tested while using hormonal contraception. Some people see small shifts while on the pill. Your doctor may interpret results with that in mind or suggest retesting after a break if decisions hinge on a borderline value.
What day of the cycle is best
Any day is acceptable because AMH is relatively stable across the month. If your cycle is irregular or you are not menstruating, you can still test. Your GP may pair AMH with other day specific blood tests for a fuller picture.
Does AMH predict menopause timing
AMH trends lower as menopause approaches, but it does not set the exact age of menopause. Very low levels in the context of symptoms can suggest perimenopause. Your doctor may combine AMH with cycle history and other hormones to guide expectations.
Is there a home AMH test in Australia
AMH requires a blood sample analysed in a lab. Some services offer at home collection kits that send samples to accredited laboratories. Discuss any kit with your GP to ensure the assay used is reliable and suited to clinical decision making.
Can endometriosis affect AMH
Endometriosis itself may not directly lower AMH, but ovarian endometriomas and surgery to remove them can reduce ovarian reserve. If you have endometriosis, an ultrasound and AMH together help assess current fertility and plan timing.
Should I repeat AMH and how often
Repeat testing is useful if the first result is unexpected for age, if labs used different assays, or if major health events occur. Many people wait six to twelve months between tests unless time sensitive decisions are underway.
Gentle next steps for your fertility journey
If AMH testing is on your mind, start with a GP appointment to discuss your goals, cycle history, and any symptoms. Your GP can arrange blood tests and ultrasound, advise on rubella and preconception screening, and refer you to a fertility specialist if needed. If you are trying to conceive now, tighten the basics that make a difference. Track your fertile window so you time intercourse with ovulation rather than guessing. Support your routine with enough sleep, steady exercise within your capacity, and a diet that suits your needs. If you would like simple tools to bring structure to each month, our accurate ovulation tests and pregnancy tests are designed to be easy to use at home. If questions come up about test choice or timing, contact us and we will point you to clear information that fits Australian care pathways. Measured steps now can save time and help you feel more in control while you put your plan in place.

References
https://www.healthdirect.gov.au/fertility-tests
https://www.healthdirect.gov.au/fertility
https://ranzcog.edu.au/womens-health/patient-information-resources/infertility
https://www.jeanhailes.org.au/health-a-z/fertility
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/infertility
https://www.health.qld.gov.au/public-health/topics/sexual-health/fertility
https://www.nswhealth.gov.au/kidsfamilies/women/fertility
https://healthywa.wa.gov.au/Articles/F_I/Fertility-and-conception


