12 min read
Dec 1, 2025
PCO vs PCOS: Differences, Symptoms & Treatments Explained
Written by
Fertility2Family Team

Medically reviewed by
Evan Kurzyp, RN (AHPRA), BSN, Master of Nursing
Polycystic ovaries seen on an ultrasound do not always mean you have polycystic ovary syndrome. Polycystic ovarian morphology describes how ovaries look on a scan, while polycystic ovary syndrome is a medical condition that affects hormones, ovulation, skin, and metabolic health. Many women learn about polycystic ovaries during a routine scan and have no symptoms at all. Others have polycystic ovary syndrome and need a plan for periods, fertility, and long-term health. Getting the right diagnosis helps you decide what to do next, whether you are trying to conceive now, planning ahead, or managing symptoms. If you are unsure which category you fit into, a GP can review your cycle history, examine you, and order targeted tests. This article explains the difference, what causes symptoms, how diagnosis works in Australia, and how ovulation and pregnancy tests fit into the picture.
Quick Answers About PCO vs PCOS
Do polycystic ovaries mean I have PCOS?
No. Polycystic ovaries are a common ultrasound finding and often occur without symptoms. Polycystic ovary syndrome is diagnosed when there are symptoms such as irregular ovulation and signs of high androgens, not just an ultrasound appearance.
Can you have PCOS with regular periods?
Yes. Some people with polycystic ovary syndrome have cycles that look regular but still show hormonal signs of the condition. A GP can check for androgen levels, ovulation patterns, and metabolic risks to confirm the picture.
Does PCOS always cause infertility?
No. Many people with polycystic ovary syndrome conceive with lifestyle measures or simple treatments. Others may need ovulation induction or assisted reproduction. People with polycystic ovaries alone usually ovulate and have good natural fertility.

What Are Polycystic Ovaries and PCOS?
Polycystic ovaries, often shortened to PCO, describe an ovary with many small follicles seen on ultrasound. These follicles are fluid-filled sacs that contain immature eggs. This pattern is common in young adults and can occur in people with regular cycles and no symptoms. In that case it is considered a normal variation.
Polycystic ovary syndrome, or PCOS, is a medical diagnosis based on symptoms and tests. Doctors look for two of three features. The first is irregular or absent ovulation, which causes irregular or widely spaced periods. The second is signs of higher androgens such as acne, extra facial or body hair, or a blood test showing high testosterone. The third is a polycystic appearance on ultrasound. Other conditions that mimic PCOS must be ruled out before a diagnosis is made.
It helps to think of polycystic ovaries as an imaging description and polycystic ovary syndrome as a hormonal and metabolic condition. You can have one without the other. Clear language during consults prevents confusion and guides the right next step.
Why PCOS Happens and How It Differs From PCO
PCOS has causes that involve genetics, insulin resistance, and how the ovaries and brain hormones communicate. Insulin resistance means the body’s cells do not respond well to insulin, and the pancreas releases more insulin to keep blood sugar stable. Higher insulin can prompt the ovaries to make more androgens, which then disrupts ovulation. This cycle can cause irregular periods, acne, hair growth on the face or body, and scalp hair thinning.
Not everyone with PCOS has insulin resistance, but it is common. Weight can interact with this pattern, although people of any size can have PCOS. Sleep, stress, and family history also play a part. Because PCOS spans hormones, metabolism, and reproductive health, care usually combines lifestyle changes and medical options.
PCO alone has none of these effects. It reflects the number and arrangement of follicles, which can be higher in young adults and often settles with age. People with PCO and regular cycles usually ovulate. If periods are regular and there are no androgen symptoms, PCOS is unlikely even if an ultrasound shows a polycystic pattern.
How PCOS and PCO Are Diagnosed in Australia
Diagnosis starts with a careful history. Your GP will ask about period timing, bleeding patterns, acne, hair changes, scalp hair loss, weight changes, and family history of diabetes or PCOS. They will check your blood pressure, weight, height, and waist, and may examine the skin for acne or dark skin patches linked to insulin resistance.
Blood tests often include total and free testosterone, sex hormone binding globulin, other androgens if needed, and screening for thyroid or prolactin problems that can also affect cycles. Doctors may check fasting glucose, an oral glucose tolerance test, and lipids to map metabolic risk. These tests help confirm the diagnosis and guide a plan.
Pelvic ultrasound can show a polycystic ovarian appearance. Ultrasound alone does not diagnose PCOS. In Australia, doctors apply accepted criteria that combine symptoms, blood tests, and imaging. Adolescents need special care because many normal features of puberty can look like PCOS. A GP can advise on timing for review and when to wait before labelling it as PCOS.

What Tests Involve and What to Expect
A standard pelvic ultrasound uses a probe across the lower belly with a full bladder, or a transvaginal probe for a closer view if appropriate. The sonographer counts follicles and measures ovarian volume. The scan takes minutes, and results go back to your GP or specialist.
Hormone blood tests are usually done in the morning. If cycles are regular, some tests are timed to the early period days. If cycles are irregular, your doctor will time them to suit your pattern. A progesterone test about seven days after suspected ovulation can confirm if ovulation occurred. If cycles are long or unpredictable, a series of tests may be planned.
An oral glucose tolerance test measures how your body handles sugar. After a fasting blood test, you drink a glucose solution, then have further blood tests. This helps detect insulin resistance and diabetes risk. These results do not just set a diagnosis. They guide practical choices on food, movement, and medicines to protect long-term health.
Managing Symptoms at Home and Lifestyle Care
Small daily changes can improve periods, ovulation, and skin. A balanced eating pattern with regular meals supports stable blood sugar. Many people find a focus on fibre-rich vegetables, whole grains, lean proteins, and healthy fats helpful. Reducing sugary drinks helps with energy dips and can smooth appetite. There is no single diet that suits everyone. Choose a plan you can keep up over time.
Movement most days supports insulin action and mood. Aim for a mix of brisk walking or cycling with simple strength work. Build up gradually and choose activities you enjoy. Quality sleep and a regular sleep routine also help regulate hunger and stress hormones. Mindfulness or other stress management can reduce stress-related flares of acne or emotional eating.
Myo-inositol is a supplement used by some people with PCOS. Evidence suggests it may support ovulation in some cases. It is not a cure. Check with your GP or pharmacist, especially if you take other medicines. If you use skin treatments for acne or hair growth, ask about safe options if you are trying to conceive or could be pregnant.
When to See a GP or Specialist in Australia
Book a GP visit if you have irregular periods, cycles longer than thirty five days, very heavy or very painful periods, or new facial or body hair. Seek care if you have acne that does not respond to pharmacy care, scalp hair thinning, or sudden weight changes. If you are under thirty five and have tried for twelve months without success, or over thirty five and have tried for six months, talk to your GP. If your cycles are irregular, ask sooner.
Your GP can manage testing and first-line care. They may refer you to an endocrinologist or gynaecologist if you need specialist input. If you plan a pregnancy, preconception advice helps address nutrients, immunisations, and medical risks. If you have prolonged bleeding, severe pelvic pain, or fainting, seek urgent care.
Some medicines used for PCOS need medical oversight. Metformin can help with insulin resistance and may improve cycle regularity. It can cause stomach upset at first. Spironolactone can help with acne and hair growth, but it can affect potassium and is not safe in pregnancy. Effective contraception is needed while taking it. Your doctor will advise on monitoring.
Ovulation and Pregnancy Tests With PCO or PCOS
Ovulation predictor kits measure luteinising hormone in urine. They suit people with regular cycles and people with PCO who ovulate predictably. In PCOS, luteinising hormone can be elevated across the cycle. This can cause false positives or repeated surges without ovulation. If your tests are confusing, swap to other methods.
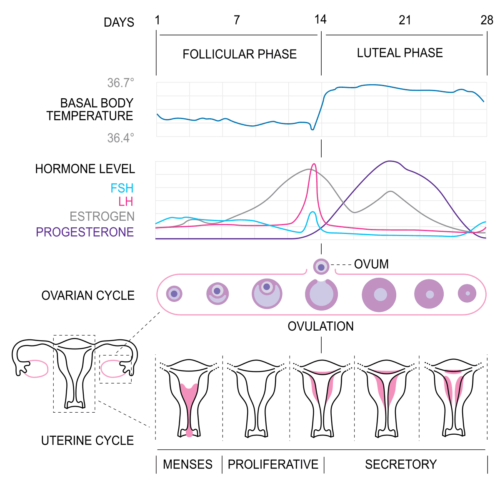
Basal body temperature tracking can show a rise after ovulation, although it does not predict it. Cervical mucus changes give helpful clues. A blood test for progesterone about a week after suspected ovulation confirms whether it happened. Ultrasound follicle tracking is another option arranged by your GP or specialist if you are actively trying to conceive.
Pregnancy tests measure hCG in urine and work the same in people with PCOS. Because cycles may be long, testing two weeks after suspected ovulation is the most reliable approach. If you are unsure when you ovulated, test if your period is late. Some fertility medicines can affect pregnancy test timing. Discuss this with your doctor if you are on treatment.

Fertility and Pregnancy Outlook for PCO and PCOS
Most people with PCO alone ovulate and do not need medical help to conceive. If cycles are regular and timed intercourse is possible, natural conception rates are good. If your cycle length varies a little, simple tracking over a few months often gives enough clarity to time intercourse.
In PCOS, ovulation can be irregular or absent. Many people conceive after lifestyle changes that improve insulin action and make ovulation more likely. If cycles remain irregular, first-line ovulation induction in Australia often starts with tablets such as letrozole. Your doctor may use blood tests and ultrasound to time intercourse and lower the chance of multiple pregnancy. If tablets are not effective, options include gonadotrophin injections or IVF under specialist care.
Early pregnancy care matters for everyone with PCOS. A GP may arrange early checks of hCG and progesterone in selected cases and plan screening for gestational diabetes. Good preconception care lays the groundwork for a healthy pregnancy and postpartum recovery.
Frequently Asked Questions About PCO and PCOS Australia
Can PCO go away on its own?
The ultrasound appearance can change over time. Many young adults have a polycystic pattern that settles with age. If your periods are regular and you feel well, no treatment is needed.
Does the oral contraceptive pill hide PCOS?
The pill can regulate bleeding and improve acne and hair growth. It can also change blood test results. Diagnosis is best made when off the pill for a period of time if it is safe for you to pause it. Ask your GP how to plan this.
Is anti-Müllerian hormone the same as a PCOS test?
AMH reflects the number of small follicles. It can be higher in PCOS but is not a stand-alone test for diagnosis. Doctors use AMH with other information rather than by itself.
Does PCOS increase miscarriage risk?
Some studies suggest a higher risk, especially with untreated insulin resistance. Preconception checks, weight management if needed, and early pregnancy care help manage risk. Most people with PCOS have healthy pregnancies.
Can I improve egg quality with lifestyle changes?
Healthy eating, regular movement, not smoking, and managing sleep and stress support overall reproductive health. No supplement can guarantee better egg quality, but a healthy routine gives the best chance for your age and medical picture.
How often should I repeat an ultrasound?
If you have stable symptoms and regular periods, you may not need repeat scans. If your symptoms change or you are starting fertility care, your doctor may repeat imaging to guide treatment.
Next Steps and How We Can Help
If your scan report mentions polycystic ovaries, start by noting your cycle dates for the next three months and any skin or hair changes. Book a GP visit if your cycles are irregular or you plan a pregnancy in the next year. Ask about hormone tests, a check for insulin resistance, and whether an ultrasound adds value at this point. If PCOS is confirmed, set one or two realistic goals you can begin this week, such as a daily walk or a regular bedtime. Small steps add up and support ovulation, mood, and long-term health.
If you are timing intercourse, at-home ovulation tests may be helpful with regular cycles or PCO without cycle disruption. If you have PCOS and find ovulation tests confusing, switch to a menstrual diary, cervical mucus observation, and GP-arranged blood tests for ovulation confirmation. Pregnancy tests work the same in PCOS, and testing two weeks after suspected ovulation is a practical approach. If you want a tailored plan, speak with your GP or a fertility specialist. Clear information, steady support, and tools that suit your cycle can make planning feel manageable.
References
https://www.healthdirect.gov.au/polycystic-ovary-syndrome-pcos
https://www.healthdirect.gov.au/ultrasound-scan
https://www.healthdirect.gov.au/insulin-resistance
https://www.healthdirect.gov.au/infertility
https://www.jeanhailes.org.au/health-a-z/pcos
https://www.jeanhailes.org.au/health-a-z/pregnancy-and-birth/trying-to-conceive
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/polycystic-ovary-syndrome-pcos
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/ultrasound-scan
https://www.monash.edu/medicine/sphpm/mchri/pcos
https://ranzcog.edu.au/womens-health/patient-information-resources