11 min read
May 2, 2026
Diarrhoea During Ovulation: Causes, Fertile Window and Care
Written by
Fertility2Family Team

Medically reviewed by
Evan Kurzyp, RN, BSN, Master of Nursing
AHPRA registration: NMW0002424871
Many people notice bowel changes across the menstrual cycle. If you get loose stools or tummy cramps right when you ovulate, it is natural to ask whether the two are connected. Ovulation is the release of an egg from the ovary. Around this time, shifts in oestrogen and progesterone can change how the gut moves. Some people pass stools more often, while others feel bloated or constipated later in the cycle. Short lived diarrhoea around ovulation is usually harmless and settles with simple care at home. Persistent pain, fever, blood in the stool, heavy bleeding or one sided pelvic pain need medical care in Australia. This guide explains why ovulation and diarrhoea sometimes occur together, what else could be going on, when to see a GP, and which tests and self care steps can help.

Quick Answers About Ovulation and Diarrhoea
Can ovulation cause diarrhoea Short bursts of diarrhoea can occur around ovulation due to hormone shifts and local prostaglandins, which influence smooth muscle in the uterus and the gut.
How long does it last For most people it lasts one to three days and improves with fluids, light food and rest. If symptoms continue beyond a few days or worsen, see your GP.
Is it a sign of pregnancy Diarrhoea at ovulation is not a reliable sign of pregnancy. Use an ovulation test to time your fertile window and a pregnancy test after a missed period.
What ovulation is and why your gut may react
Ovulation happens mid cycle when a mature egg is released from an ovary and enters the fallopian tube. Oestrogen rises before ovulation, then progesterone rises after the egg is released. These hormones coordinate cervical mucus, basal body temperature and the uterine lining. They also influence the gut. Prostaglandins are natural lipid messengers made in many tissues, including the reproductive tract. Around fertile days, local prostaglandins help the follicle rupture and can affect nearby smooth muscle. In some people this speeds bowel movement and leads to softer stools.
Not everyone notices the same pattern. Some feel mild lower abdominal cramps with clear stretchy cervical mucus and a short spell of loose stools. Others swing the other way and feel more constipated later in the luteal phase when progesterone is higher. Tracking body signs, including cervical mucus and basal body temperature, helps link symptoms to cycle timing. If you are learning your pattern, our Australian Fertility Kits can support cycle tracking alongside a symptom diary.
Causes of diarrhoea around ovulation
Hormonal change is the most common reason for bowel shifts at mid cycle. Rising oestrogen and local prostaglandins can increase gut motility in sensitive people. A sudden food trigger, caffeine, alcohol, or a change in routine can add to this and tip the balance toward loose stools. Some people with irritable bowel syndrome have a gut that is more reactive to hormone fluctuation. Their bowel can speed up during the fertile window, then slow down later, which can cause alternating diarrhoea and constipation across the cycle.
Pelvic conditions may also be involved. Endometriosis can cause pain that flares with ovulation and periods. If endometrial tissue sits on the bowel surface, bowel movements can be painful and erratic. A gut infection can be present by chance at the same time as ovulation. Food intolerances such as lactose or fructose malabsorption can look like cyclical diarrhoea if the timing lines up with diet changes. Very rarely, severe one sided pelvic pain with light headedness and unusual bleeding could be an ectopic pregnancy. While ectopic pregnancy is not caused by ovulation diarrhoea, it can overlap in timing and needs urgent care if suspected.
How your GP in Australia may assess the problem
Most people can start with self care. If symptoms are frequent, severe or keep you from daily activities, book a standard GP appointment. Your GP will ask about your menstrual cycle, timing of symptoms, stool frequency, recent travel or illness, diet, medications and pregnancy plans. They may ask you to keep a symptom diary for at least two cycles that notes bowel habits, pain scores, mucus changes, ovulation test results and any triggers such as food or stress.
Based on your history, your GP may check for dehydration, abdominal tenderness and pelvic signs. If there are red flags such as fever, blood in stool, persistent vomiting, heavy bleeding, severe lower abdominal pain or shoulder tip pain, your GP will arrange urgent tests or refer you to hospital. If endometriosis or irritable bowel syndrome is suspected, a referral to a gynaecologist or a gastroenterologist may be offered. Healthdirect can provide triage advice after hours and guidance on when to seek urgent care.
Tests that may be recommended and what they involve
Pregnancy testing is often the first step if there is any chance of conception. A urine pregnancy test is quick. A blood test for beta hCG confirms and dates an early pregnancy. If there is concern about an ectopic pregnancy, blood tests are repeated and an ultrasound is arranged. A pelvic ultrasound, often transvaginal, uses sound waves to view the uterus and ovaries and does not require radiation. It can suggest ovarian cysts or features that may align with endometriosis, although laparoscopy is the only way to diagnose endometriosis with certainty.
To assess bowel causes, your GP may order stool tests to look for infection, blood or inflammation. Blood tests can check iron levels, signs of inflammation and coeliac disease. If lactose or fructose intolerance is suspected, a breath test may be arranged through a specialist clinic. Faecal calprotectin can help tell irritable bowel syndrome apart from inflammatory bowel disease. Colonoscopy is rarely needed in younger people without red flags. If symptoms match a cyclical hormone pattern, formal tests may be limited to ruling out pregnancy and infection, while management focuses on timing and lifestyle steps.
Practical ways to manage symptoms at home
Most episodes settle with gentle care. Sip fluids through the day and include an oral rehydration solution if stools are very watery. Plain foods such as rice, bananas, oats and toast can be easier to tolerate while your gut settles. Many people feel better with small frequent meals rather than large servings. Limit very spicy foods, alcohol and large amounts of caffeine on your peak fertile days if these are personal triggers.
Soluble fibre can help steady bowel movements. Oats, psyllium husk and cooked vegetables are useful options. Increase fibre slowly and drink water to avoid gas and cramping. Yoghurt or kefir with live cultures can support gut bacteria. Fermented foods such as sauerkraut or kimchi can be helpful if you tolerate them. Some people find calcium rich foods such as dairy or fortified alternatives settle muscle cramps, including gut cramps. If you use loperamide for short term control, follow the pack advice and avoid if you have fever, blood in the stool or severe abdominal pain.
Regular movement such as walking, yoga or swimming can ease gut tension. Good sleep and simple breathing exercises can reduce the stress response that often sparks bowel urgency. If irritable bowel syndrome is present, a dietitian can guide a short trial of a low FODMAP approach, then reintroduction to identify triggers. Keep your plan simple and personalised, and return to a normal balanced diet once the flare settles.
Where ovulation and pregnancy tests fit into the picture
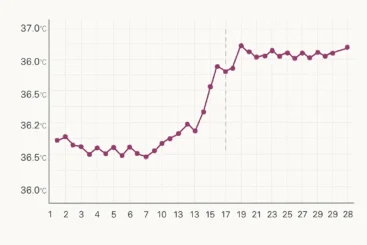
Ovulation does not cause diarrhoea in everyone, yet bowel changes can mark your fertile window. Ovulation predictor kits detect the surge in luteinising hormone that occurs one to two days before the egg is released. A positive test confirms timing even if bowel symptoms blur the picture. Cervical mucus and basal body temperature can add context. Many people test for LH in the late morning or afternoon and take their temperature on waking each day, then review the pattern across a cycle.
Diarrhoea does not directly affect urine based tests. Heavy fluid intake can dilute urine and make a faint LH or pregnancy test harder to read. If you are very thirsty because of diarrhoea, avoid over drinking right before testing. A pregnancy test is best if your period is late. If you have strong pain on one side, shoulder tip pain, heavy bleeding or feel dizzy, seek urgent assessment before relying on a home test. Learn more about timing and tools with our Australian Fertility Kits .
When to see a GP or specialist in Australia
Book a GP visit if diarrhoea lasts longer than three days, keeps returning every cycle, or is severe enough to limit work or study. Seek care if you have fever, blood or mucus in the stool, dehydration that does not improve with oral fluids, or weight loss. See your GP if pelvic pain is getting worse over time or intercourse is painful. If periods are very heavy or you have bowel pain that matches your cycle, ask about endometriosis. If you could be pregnant and you have lower abdominal pain on one side, shoulder tip pain, fainting, or heavy bleeding, go to the nearest emergency department or call triple zero. Healthdirect can advise on next steps if you are unsure.
In ongoing cases, your GP may refer you to a gynaecologist to assess ovulation and pelvic causes, or a gastroenterologist to review bowel symptoms. A dietitian can help with meal planning and fibre choices. Many people do well with a mix of cycle tracking, targeted diet changes and reassurance. Care is individual, and most people do not need complex tests.
Frequently Asked Questions About Ovulation and Diarrhoea Australia
Does diarrhoea at ovulation affect fertility Short term bowel changes do not reduce your chance of conceiving. Focus on timing intercourse in the fertile window, staying hydrated and resting if you feel unwell.
Can period pain tablets help mid cycle Simple pain relief such as paracetamol can help cramps. Anti inflammatory tablets can help some people but may not suit those trying to conceive, so check with your GP or pharmacist.
Is it normal to have nausea as well Mild nausea can occur with hormone shifts at mid cycle. If vomiting persists, you cannot keep fluids down, or there is severe pain, seek medical care.
Do probiotics work for cyclical diarrhoea Some people feel better with yoghurt, kefir or a probiotic supplement. Effects vary. Give any new product two to four weeks and stop if symptoms worsen.
Can I exercise on ovulation days if I have diarrhoea Light activity is fine and can ease cramps. Avoid very intense sessions while dehydrated. Rehydrate and return to normal training once stools settle.
What if I also have constipation later in the cycle This pattern is common. Oestrogen can speed things up near ovulation. Progesterone can slow things down in the luteal phase. Aim for steady fibre and fluids across the whole cycle.
Taking the next step
Short lived diarrhoea during ovulation is common and usually settles quickly. Understanding your cycle helps you plan your week, reduce worry and time intercourse or insemination when it counts. If a pattern emerges, keep a simple diary that notes your period start date, ovulation signs, bowel habits and any triggers such as food, stress or lack of sleep. Small steps make a difference. Drink enough water, choose soluble fibre, add live cultured yoghurt or kefir if you tolerate dairy, and rest if cramps flare.
If you are trying to conceive, pairing body signs with testing can give you clarity. Ovulation tests confirm your fertile window and pregnancy tests help you check in after a missed period. Tools are only part of the picture. If symptoms persist or you are worried, your GP can help you rule out infection, food intolerance, irritable bowel syndrome or pelvic causes such as endometriosis. With the right plan, most people feel better within days and can keep moving toward their goals with confidence. If you want simple ways to track fertile days, our Australian Fertility Kits can support your routine alongside medical advice.
Last reviewed: May 2, 2026
Next scheduled review: Mar 2027
References
Fertility2Family publishes Australia-focused fertility education. Articles are written by our team and medically reviewed by Australian-registered health practitioners. We use Australian consumer medicine information, Australian clinical and public health guidance, and peer-reviewed research consistent with Australian care. We explain what the evidence suggests, what it cannot confirm, and when to see a GP or fertility specialist. Each article lists its author, medical reviewer, and review dates.
https://www.healthdirect.gov.au/ovulation
https://www.healthdirect.gov.au/diarrhoea
https://www.jeanhailes.org.au/health-a-z/periods/menstrual-cycle
https://www.jeanhailes.org.au/health-a-z/gastrointestinal/gut-health
https://www.healthdirect.gov.au/endometriosis
https://www.racgp.org.au/afp/2017/july/irritable-bowel-syndrome-in-general-practice
https://www.healthdirect.gov.au/pregnancy-tests
https://www.health.qld.gov.au/news-events/news/ibs-symptoms-diagnosis-treatment
https://www.ranzcog.edu.au/womens-health/patient-information-resources/endometriosis-and-pelvic-pain